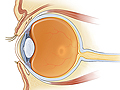
Retinal Detachment
Condition Basics
What is retinal detachment?
Retinal detachment is an eye problem that happens when the retina, a thin membrane of nerve tissue that lines the back of the eye, comes off (detaches).
The nerve cells in the retina normally detect light entering the eye and send signals to the brain about what the eye sees. But when the retina detaches, it no longer works as it should. It can cause blurred and lost vision. Retinal detachment requires medical care right away.
What causes it?
Retinal detachment is caused by:
- Tears or holes in the retina. A tear in the retina is the most common cause of retinal detachment. These tears can happen when fluids collect under the retina. Tears can also be caused by posterior vitreous detachment (PVD), when the vitreous gel shrinks and separates from the retina. An eye or head injury or other eye disorders may also cause these tears or holes.
- Traction on the retina . If tissue builds up between the vitreous gel and the retina, it can pull the retina away from the back of the eye. The pulling is called traction.
- Fluid buildup under the retina. This fluid buildup can cause the retina to come off the back of the eye. Fluid buildup may be caused by inflammation or disease in the retina, in the layer just beneath the retina (choroid), in blood vessels, or in tissues in the eye.
What are the symptoms?
Many people see floaters and flashes of light before they have symptoms of retinal detachment. Floaters are spots, specks, and lines that float through your field of vision. Flashes are brief sparkles or lightning streaks that are easiest to see when your eyes are closed. They often appear at the edges of your visual field. Floaters and flashes don't always mean that you will have a retinal detachment. But they may be a warning sign, so it's best to be checked by a doctor right away.
In rare cases, a retinal detachment happens without warning. The first sign of detachment may be a shadow across part of your vision that doesn't go away. Or you may have new and sudden loss of side (peripheral) vision that gets worse over time.
How is it diagnosed?
To diagnose retinal detachment, your doctor will ask you questions about your symptoms. You will be asked about your past eye problems and risk factors. The doctor will also test your near and distance vision (visual acuity) and side (peripheral) vision. These routine vision tests don't find retinal detachment itself. But they can find problems that could lead to or result from retinal detachment.
A doctor can usually see a retinal tear or detachment while checking the retina using ophthalmoscopy. This test allows the doctor to see inside the back of the eye using a magnifying tool with a light.
If a retinal tear or detachment involves blood vessels in the retina, you may have bleeding in the middle of the eye. In these cases, your doctor can view the retina using ultrasound or optical coherence tomography. These are tests that use sound or light waves to see the retina.
How is retinal detachment treated?
Surgery is the only way to reattach the retina. There are many ways to do the surgery. They include using lasers, air bubbles, or a freezing probe to seal a tear in the retina and reattach the retina. This condition needs treatment right away. Without treatment, vision loss can become severe.
What kind of surgery is done for it?
Surgery is the only way to reattach the retina. There are many ways to do the surgery. They include:
- Pneumatic retinopexy.
-
The doctor injects a gas bubble into the eyeball. The gas bubble lightly presses the detached retina to the wall of the eye. The eye doctor then uses a freezing probe or laser to seal the tear.
- Scleral buckling surgery.
-
The doctor places a piece of silicone sponge, rubber, or semi-hard plastic on the outer layer of your eye and sews it in place. This relieves pulling on the retina and prevents tears from getting worse.
- Vitrectomy.
-
The doctor removes the vitreous gel from the eye. This gives the doctor better access to remove scar tissue from the retina, repair holes, and push the retina back onto the wall of the eye.
Related Information
Credits
Current as of: October 1, 2025
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: October 1, 2025
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.